Msts score
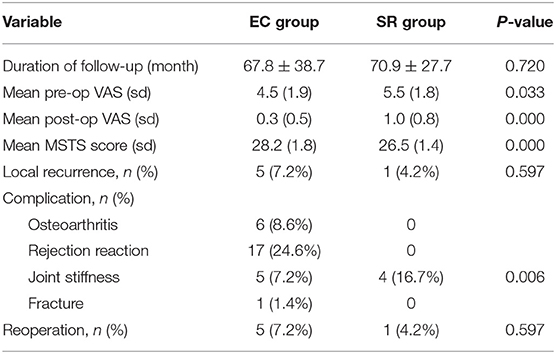
The MSTS Rating Scale is a widely used functional instrument which was developed in 1983 and later modified by the MSTS in 1993. In this perspective, it is necessary to develop a disease-specific instrument for patients with extremity sarcoma to determine their perceived physical and mental health.Ĭurrently, several disease-specific instruments have been used to evaluate the functional outcome of patients with extremity tumors, such as Musculoskeletal Tumor Society (MSTS) rating scale and the Toronto Extremity Salvage Score (TESS). Therefore, it is very important to apply the most suitable treatment for each patient. It is noteworthy that patients with sarcoma may have a significant heterogeneity regarding individual factors, such as age, financial capacity and nature of the tumor. Other disadvantages of limb-salvage surgery include the increased risk of infections and breakages of the prosthesis. By contrast, limb-salvage surgery may result in long period of hospitalization and not optimally functioning outcome. Depending on the location and the progressive status of the sarcoma, amputation surgery may still be necessary, despite at the cost of compromised body image. Recently, with the development of adjuvant therapies in the form of radiation therapy and chemotherapy, more patients had the opportunity to undergo limb-salvage surgery. Previously, patients with extremity sarcoma were routinely treated by amputation surgery. Sarcoma is a rare type of cancer that most frequently in the long bones and soft-tissue of the extremity. Through application of the Chinese MSTS, we demonstrated that patients receiving limb-salvage surgeries may have better functional outcome and QoL than those undergoing amputation surgeries. The Chinese MSTS scoring system is a reliable and valid instrument with well-accepted psychometric properties. The factor analysis indicated a 1-factor model with acceptable goodness of fit. 23.5 ± 6.3, p = 0.005), which indicated a good discrinimant validity of the Chinese MSTS. Patients undergoing amputation surgery had remarkably lower MSTS score than patients undergoing limb-salvage surgeries (18.8 ± 5.4 vs. The test for internal consistency showed a Cronbach’s α of 0.86 for the MSTS. The ICC was 0.91 (95% confidence interval (CI) = 0.85–0.96) for the test-retest reliability and 0.90 (95% CI = 0.86–0.93) for the inter-observer analysis. The construct validity was evaluated with the factor analysis. The discriminant validity was evaluated through comparison of the MSTS score between patients undergoing amputation surgeries and those undergoing limb-salvage surgeries.
The internal consistency was evaluated by Cronbach’s α, with a value >0.70 considered acceptable. The inter-observer and test-retest reliability was analyzed with intra-class correlation coefficient (ICC). The reliability of Chinese MSTS was evaluated through test-retest analysis, inter-observer analysis and internal consistency. Assessment of psychometric properties was carried out through reliability and validity test. All the patients completed the clinical assessment with the Chinese MSTS and the Chinese Toronto Extremity Salvage Score (TESS). MethodsĪ cohort of 98 patients who had undergone surgery for lower extremity sarcoma were included. This study aims to investigate the reliability and validity of the Chinese version of the MSTS, and to evaluate functional outcomes of the surgical treatment of lower extremity sarcoma using the Chinese MSTS. There were no differences in functional outcomes when comparing distal femur endoprostheses with proximal tibia endoprostheses.The Musculoskeletal Tumor Society (MSTS) scoring system is a disease-specific instrument to determine the physical and mental health for patients with extremity sarcoma. We conclude that endoprosthesis replacement for primary bone tumours had early good to excellent functional outcome. Three deep infections required early, two-stage revision and resulted in poor MSTS scores. The mean MSTS score for both DF and PT endoprosthesis together was 21.13 (70.43%), and The MSTS scores for DF was 21.94 (73.13%) and PT was 19.75 (65.83%) Infection developed in 7 cases and 5 of which were PT endoprosthesis cases. Primary tumours were classified as follows: 33 osteosarcoma, 20 stage III giant cell tumour (GCT) and one case of mesenchymal chondrosarcoma. The study sample included 34 cases of distal femur and 20 cases of proximal tibia endoprosthesis replacement. We used the Musculoskeletal Tumour Society Scoring System (MSTS) for functional evaluations to compare differences between distal femur (DF) and proximal tibia (PT) placements. We evaluated functional outcomes for patients who underwent surgery for resection and endoprosthesis replacement for primary tumours around the knee.
